6. Effective communication.
-
Communication concepts.
Communication is important when dealing with others. How you communicate will affect how others feel and behave, which, in turn, can make your job difficult or easy. Learning how communication happens and some basic techniques will enable you to provide better care to your client. Communication is the process of sending and receiving a message. It consists of verbal and non-verbal communication. Verbal communication has to do with words, whether they are written, read, or said aloud. Words should be simple and clear so that people understand correctly. Remember that words may have different meanings to different people. Non-verbal communication, more commonly called ‘body language,’ sends a message too. We send messages with our facial expressions, tone of voice, gestures, posture, eye contact, and touch. Communication is misunderstood when the verbal and non-verbal (body language) messages are different. If you say one thing and your body is sending a different message, people get confused. Most people, when they get conflicting messages, will believe what they see. You have probably heard the phrase “actions speak louder than words.” That really applies in this situation. You need to be aware of your own body language as well as others.’
Communication concepts
Principles of positive communication.
Types of communication
Communication involves the imparting or interchanging thoughts, opinions, or information among people by speech, writing, or signs. People communicate in different ways. How effective is your communication style? Are you giving away thoughts you don’t mean to?
Verbal
Verbal communication entails the use of words in delivering the intended message. The two major forms of verbal communication include written and oral communication.
Written communication includes traditional pen and paper letters and documents, typed electronic documents, e-mails, text chats, SMS and anything else conveyed through written symbols such as language. This type of communication is indispensable for formal business communications and issuing legal instructions.
Communication forms that predominantly use written communication include handbooks, brochures, contracts, memos, press releases, formal business proposals, and the like. The effectiveness of written communication depends on the writing style, grammar, vocabulary, and clarity
Oral/Verbal Communication
The other form of verbal communication is the spoken word, either face-to-face or through phone, voice chat, video conferencing or any other medium. Various forms of informal communications such as the grapevine or informal rumor mill, and formal communications such as lectures, conferences are forms of oral communication. Oral communication finds use in discussions and causal and informal conversations. The effectiveness of oral conversations depends on the clarity of speech, voice modulation, pitch, volume, speed, and even non-verbal communications such as body language and visual cues.
Verbal communication makes the process of conveying thoughts easier and faster, and it remains the most successful form of communication. Yet, this makes up only seven percent of all human communication!
Nonverbal Communication
Nonverbal communication entails communicating by sending and receiving wordless messages. These messages usually reinforce verbal communication, but they can also convey thoughts and feelings on their own.
Physical nonverbal communication, or body language, includes facial expressions, eye contact, body posture, gestures such as a wave, pointed finger and the like, overall body movements, tone of voice, touch, and others.
Facial expressions are the most common among all nonverbal communication. For instance, a smile or a frown conveys distinct emotions hard to express through verbal communication. Research estimates that body language, including facial expressions, account for 55 percent of all communication.
Paralanguage
The way something is said, rather than what is actually said, is an important component of nonverbal communication. This includes voice quality, intonation, pitch, stress, emotion, tone, and style of speaking, and communicates approval, interest or the lack of it. Research estimates that tone of the voice accounts for 38 percent of all communications.
Other forms of nonverbal communication usually communicate one’s personality. These include:
- Aesthetic communicationor creative expressions such as dancing, painting, and the like.
- Appearance or the style of dressing and grooming, which communicates one’s personality.
- Space language such as paintings and landscapes communicate social status and taste.
- Symbolssuch as religious, status, or ego-building symbols.
Visual Communication
A third type of communication is visual communication through visual aids such as signs, typography, drawing, graphic design, illustration, color and other electronic resources.
Visual communication with graphs and charts usually reinforces written communication, and can in many case replace written communication altogether. As the adage goes “a picture is worth a thousand words”; such visual communication is more powerful than verbal and nonverbal communication on many occasions. Technological developments have made expressing visual communications much easier than before.
A good understanding of the different types of communication and communication styles can help you know and deal with people better, clear up misunderstandings and misconceptions, and contribute to the success of the enterprise.
-
Communication techniques and guidelines.
Everything you do or say communicates a message.
Good communication skills are essential. Speaking, listening, feedback and actions are important for everything a PCW does:
- providing proper care, following directions
- showing concern, building trust
- getting along with residents, families, visitors, and co-workers reducing conflict, solving problems
- reporting observations, giving clear messages
- listening, not interrupting or judging
- explaining procedures, resolving concerns
- building relationships
Communication simply means sending and receiving messages. However, effective communication involves more than words. Both verbal and nonverbal messages carry meaning.
Verbal. Words. Use simple and clear words.
Nonverbal. Body language. Everything you do sends a message:
- facial expressions;
- gestures;
- the tone of voice;
- posture;
- eye contact;
- silence touch.
Verbal and nonverbal language must agree in order to send clear messages. The problem is that most people are not aware of their nonverbal behavior. Unless verbal and nonverbal language agree, the listener gets a mixed message. For example, if the PCW expresses care and concern, but stands with folded arms and a look of disgust, the client gets conflicting messages. Unfortunately, when messages are mixed, the nonverbal impressions speak louder than the words.
Communicate as clearly as possible to avoid any confusion. Medical abbreviations are important for PCWs lo know in order to understand instructions. But do not use abbreviations when you are talking with the clients or their families. Use words that are easily understood.
Listening
Active listening takes effort, self-control, and practice. Pay attention to what the other person is saying, and fight the tendency to think about your reply while the other person is talking. Avoid interrupting or finishing someone else’s sentences. Teach yourself to be patient and wait for your tum to talk.
Clients need to feel listened to, heard, and understood. Listen for facts and listen to feelings. Ask questions when you do not understand. Being a good listener helps the PCW learn what the client likes and doesn’t like, as well as problems, concerns, interests, and needs.
Feedback
Words have different meanings to different people, which can lead to misunderstandings. Feedback is a process to avoid confusion and to clear up any misunderstanding.
To be sure that you understand what others say to you, paraphrase (repeat what you heard using your own words). Ask if the statement is correct. Check whether others understand what you are saying by asking questions and encouraging feedback.
Guidelines for Effective Communication
Open your heart to the clients, and try to understand their problems, pain, and frustrations. Try to imagine what it is like to be in their situation. Take time to smile and say “hello.” Convey warmth, understanding, and interest. Small acts of kindness can brighten someone’s day.
Communicate with people at their level of under standing. Use an appropriate manner, level, and pace according to individual abilities.
- Take time to listen.
- Be patient, and show respect.
- Think before you speak.
- Be aware of your body language.
- Speak clearly, and use a friendly tone.
- Use simple words and short sentences.
- Ask open questions (e.g., “how?” or “why?”).
- Paraphrase (summarize in your own words).
- Ask for clarification.
- Be alert to key words about feelings (e.g., “guilt” or “hurt”), and ask for more information.
- Avoid criticizing or judging.
- Do not interrupt.
Good communication skills build positive relation ships. Keys to maintaining good relationships include kindness, caring, and understanding.
Good Communication Techniques
- Listening: Take the time to listen. Pay attention to what others are saying and ask questions. Always communicate what you are doing with the care recipient. Do not work in silence.
- Be patient: Give others the time to say what they want.
- Eye contact: Look at the person and focus on what he/she is saying. Listen with interest.
- Body Language: Be aware of facial expressions and tone of voice. Watch others for differences between verbal and non-verbal messages.
- Keep conversations and words simple and clear.
- Use feedback: Repeat what you heard in your own words.
- DO NOT do the following:
- Argue with anyone;
- Interrupt a conversation;
- Appear bored or impatient;
- Pass judgment or give advice;
- Threaten or use harsh language;
- Be defensive – (It is better to be open to suggestions).
Barriers to communication.
There are many reasons why interpersonal communications may fail. In many communications, the message (what is said) may not be received exactly the way the sender intended. It is, therefore, important that the communicator seeks feedback to check that their message is clearly understood.
The skills of Active Listening, Clarification, and Reflection may help but the skilled communicator also needs to be aware of the barriers to effective communication and how to avoid or overcome them.
There are many barriers to communication and these may occur at any stage in the communication process. Barriers may lead to your message becoming distorted and you, therefore, risk wasting both time and/or money by causing confusion and misunderstanding. Effective communication involves overcoming these barriers and conveying a clear and concise message.
Common Barriers to Effective Communication:
A skilled communicator must be aware of these barriers and try to reduce their impact by continually checking to understand and by offering appropriate feedback.
- The use of jargon. Over-complicated, unfamiliar and/or technical terms.
- Emotional barriers and taboos. Some people may find it difficult to express their emotions and some topics may be completely ‘off-limits’ or taboo.
- Lack of attention, interest, distractions, or irrelevance to the receiver.
- Differences in perception and viewpoint.
- Physical disabilities such as hearing problems or speech difficulties.
- Physical barriers to non-verbal communication. Not being able to see the non-verbal cues, gestures, posture, and general body language can make communication less effective.
- Language differences and the difficulty in understanding unfamiliar accents.
- Expectations and prejudices which may lead to false assumptions or stereotyping. People often hear what they expect to hear rather than what is actually said and jump to incorrect conclusions.
- Cultural differences. The norms of social interaction vary greatly in different cultures, as do the way in which emotions are expressed. For example, the concept of personal space varies between cultures and between different social settings.
- Physical and emotional condition changes.
-
Communication with clients who are getting older.
The body changes with age:
This section looks at body changes. You will also learn about the changes to specific body systems and you will gain some useful information about how to provide quality care for clients who are getting older.
Visible changes.
Many visible changes take place with age. People grow shorter as the vertebrae may compress on to each other (the spinal column compresses). The density of bones decreases, mostly in women. Muscle tone and size decrease, the tendons become less flexible and cartilage deteriorates. These changes can cause a loss of flexibility and strength, changing the overall shape of a person’s body. Wrinkles, drier skin, decreased amounts of scalp hair and a reduction in the level of pigmentation in the skin are all common in the elderly. The skin also becomes less elastic; in other words, it doesn’t have as much stretch as younger skin. An older person’s skin gets thin, making it easier to bruise, scratch or tear. Older people perspire less, hair becomes gray and the finger and toenails grow more slowly, showing some discoloration and lines.
Sensory changes.
Many sensory changes occur with aging. Hearing loss occurs. Sounds in the higher frequency range (such as high-pitched voices) are lost first, and sounds must be louder to be heard. Hearing problems can contribute to isolation, anxiety and depression in the older adult and can result in behavior problems. The client may withdraw from gatherings rather than strain to listen.
As a direct care staff person, communicating with clients who suffer from a hearing loss can be difficult, but using the following ideas will make your job easier:
- Make sure that if clients wear hearing aids, they are in and the batteries are working.
- If they don’t wear a hearing aid you can do the following to communicate:
- Face the person and get their full attention before you talk.
- Decrease noises.
- Speak clearly and slowly.
- Speak at a lower pitch or your normal pitch.
- Use pleasant facial expressions and gestures.
- Remove gum and candy from your mouth.
- Keep your hands away from your face in case they follow your lips to understand what you are saying.
- Allow time between sentences and rephrase sentences if necessary.
- Use a pad of paper to write notes.

Vision, like hearing, is another common change in older adults. Normal changes in vision include the lack of ability to see close and read. Larger print is helpful. Older persons also do not see as well at night. In general, older adults see better with twice the light that they may have needed in the past. If the light seems very bright to you, it may be just at the limit of what the older person needs to be able to see. Make sure to avoid glare however, as this will interfere with vision too.
Sensitivity to smell and taste decreases with age. Older persons cannot taste foods the way they used to taste. This can lead to less interest in eating. If an older adult client has less pleasure when eating, this may affect what he/she eats. An older person may have a reduced appetite and weight loss. If he/she is not getting the proper nutrition it may affect other body functions such as healing of wounds. Not all taste abilities decline at the same rate. The sensitivity to the taste of salt does not decrease as much as sensitivity to some other tastes, such as too sweet foods. The concern here is that this can lead to clients eating more salt than they need, and this can lead to excess fluid retention.
The sense of touch changes. In older adults, the sense of touch may decrease as skin loses sensitivity. Pressure, pain, cold and heat do not feel the same as they used to feel. Decreases in touch sensitivity may cause clients to drop things. An older adult client may not notice the temperature of the water, so he/she can get burned more easily. You may find that you must frequently check the temperature of things before a client comes into contact with them. As a direct care staff person, watch for skin discoloring that is white or purple in color, open areas and for skin that is cooler to the touch.
Cardiovascular system. This system includes the heart, lungs and blood vessels. Circulation of the blood slows down; this can result in older clients feeling cold, especially in the hands, feet, and legs. Cuts and tears to the skin may take longer to heal and require extra care. One suggestion or guidance you can provide is to encourage the client to change positions so they are not always lying down or sitting. This will help avoid skin breakdown and increase circulation. However, be sure that changes in position are done slowly so as not to cause the client to get dizzy and fall.
Neurological system. This system includes the brain and nerve system. Cells in the brain that are lost do not reproduce, and up to 25% of brain mass can be lost in the aging process. Older people take longer to remember things, respond to questions and finish certain kinds of tasks. It is not a sign of less intelligence. Rather, it simply takes longer to make the connections in the brain than it did when the client was younger.
Respiratory system. This system that keeps us breathing changes with age, too. It takes longer to get better after a cold or flu. It is important to watch for and report shortness of breath and swelling in the legs or feet.
Urinary system. Prostate infections (in men) and infections in the bladder may increase, and recovery is slower. As a direct care staff person, to reduce the risk of bladder infections, teach the female client to wash her private area from front to back. Watch how much the client drinks (ideally, he/she should drink eight large glasses of water a day). Encourage the client to use the toilet every two hours to reduce the risk of accidents and infections. Watch for dark, foul-smelling urine and increased urinary frequency. These may be signs of a urinary tract infection that can cause pain, burning, increased confusion and behavior problems. Report any changes in urine or toileting to your supervisor.
Digestive system. This system breaks down food. Changes in the teeth and loss of teeth occur more with the elderly and can have an impact on the ability to chew and digest food. If the teeth are not strong, soft food may be easier to chew. The client may need to drink more to help swallow.
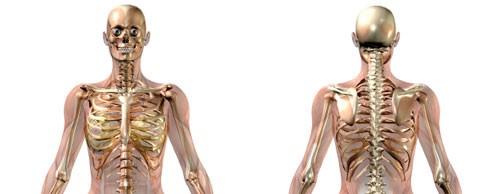
Muscular-skeletal system. A client’s muscles may be weaker, joints may be sore and stiff and bones may be brittle. As a direct care staff person, you may have to assist the client in getting in and out of a chair and with activities such as dressing and walking. Encourage the client to do simple exercises to keep limber. Walking and simple exercises are excellent activities to prevent stiffness and pain.
Psychological issues and aging:
Older people must make many adjustments. Often these adjustments are handled without any problem and the quality of life stays high. Less often, people struggle, and in some cases experience stress that reduces their quality of life. Older persons may feel afraid, confused, nervous or helpless. Generally, these reactions happen when there is a sudden and unusually negative change in a person’s life situation. When you observe any of these reactions, report them to your supervisor immediately.
It is normal for any of us to be temporarily depressed over a loss, and this is true for an older adult. Over time we adjust and this situational depression lifts. However, depression that continues without improvement is not a normal part of aging, and it can be quite serious. People who are depressed have a much higher risk of suicide. Because depression is treatable, it is important to recognize its symptoms and report them to a supervisor who can arrange for an assessment.

The symptoms for depression include sadness, guilt, a sense of worthlessness, hopelessness, fatigue, tearfulness, weight loss, irritability, excessive complaints of aches and pains that have no apparent cause, anger, and sleep disturbances. One of the things that make it harder to recognize depression is that it can often occur with other diseases or conditions such as dementia, heart disease, Parkinson’s disease, stroke, diabetes, and cancer. When this happens it is easy for people to assume that it is normal for someone with one of these conditions to be depressed. This is dangerous thinking and is not true. Despite having another illness, someone who is depressed should be treated for depression along with treatment for other illnesses.
-
Observing, Reporting and Charting.
Carefully observe each client throughout your daily contacts.
Personal Care Worker need to be alert to problems or changes in each client’s physical or emotional condition. Follow agency procedures for what to report immediately and what to report in writing. Accurate, thorough, and timely records of care and observations of each client are critical.
All information is confidential, and records must be safely stored when not in use. Some facilities keep handwritten records, and other facilities use computerized systems.
The HIPA A* Privacy Rule provides federal protection for personal health information. All records (written or electronic) are confidential. As a health team member, it is critical that you understand the facility policies regarding the safekeeping and privacy of all records.
- Health Insurance Portability and Accountability Act
Everything in the chart is confidential.
Keeping the information confidential is
your responsibility legally, ethically, and morally.
Observing
Observe each client throughout your daily contacts. Being a skilled observer helps prevent serious problems and earns the respect of the team staff. Being alert to the client and the environment reduces safety hazards and health problems. Careful observation increases your awareness of each client’s physical, emotional, and social needs.
Learn to recognize signs and symptoms of common diseases and conditions. Detecting problems in their early stages is critical. Trust your instincts. If something seems wrong, report it.
Be alert to emotional changes:
- Mood swings, loss of control
- Depressed, hopeless, crying, tearful
- Angry, difficult, irrational, agitated
- Disoriented, confused
- Anxious, frightened, pacing, restless
- Decreased or increased functioning (e.g., pulse, breathing, elimination)
- unconscious, weak, dizzy, drowsy
- Shaking, trembling, spasms.
- Chest pains.
- Cold, pale, clammy, chills.
- Hot, burning, sweating, feverish.
- Nausea, vomiting odor.
- Diarrhea, constipation.
- Excessive thirst, change in appetite.
- Change in skin color.
- Ringing in the ears.
- Blurred vision.
Be alert to physical changes:
- Swelling, edema rash, hives, blisters;
- Choking, coughing, wheezing, sneezing shortness of breath;
- Red or irritated areas, pus, drainage.
- Change in activity level weakness on one side.
Reporting
Thorough and accurate reports are made to the nursing staff as often as the resident’s condition requires. End-of-shift reports to the oncoming staff provide the information necessary for continued good care. Follow facility procedures.
-
Communication skills with impaired elders.
How do I communicate with impaired elders? As a personal caregiver, you may provide care to a client who has physical disabilities or impairments that may interfere with communication. The following are some techniques to use in those situations.
Blind or Visually Impaired Elder
- Get the personalized attention before talking.
- Identify yourself when entering the room.
- Say their name.
- Use common sounds, such as ringing a bell, whistling, etc.
- Explain what you are doing as you do it.
- Ask for feedback to check for understanding.
- Make sure eyeglasses have up-to-date prescriptions and are clean.
- Print in big, bold letters when necessary.
Deaf or Hearing Impaired Elder
- Make sure you face the client who reads lips.
- Use visual actions to communicate.
- Get their attention before talking to them.
- Face them when you are talking. Maintain eye contact; avoid turning or looking away while you are talking.
- Talk at a normal pace.
- Raise your voice some and lower your tone. DON’T yell. Speak to the side where hearing is best.
- If necessary, use paper and pencil to write messages.
- Get rid of other noises – TV, radio, etc.
- Make sure hearing aids are working and are properly inserted.
- Write down messages.
- Ask for feedback to determine to understand.
Speech Impaired, Aphasic Elder (Aphasia-Trouble speaking or understanding, often result of a stroke)
- Address the person by name.
- Keep communication simple and clear. Speak slowly and use simple words.
- Ask questions that can be answered with yes or no.
- Make message clear, emphasizing keywords, limiting details.
- Eliminate unnecessary background noises (to help the client concentrate on what is being said).
- Be patient. Give the client enough time to respond to you. At least 10 seconds is the recommendation. (Time yourself for 10 seconds so you can see how long it is. You’ll be surprised!)
- Use visual devices like a message board, pictures, or gestures.
- Be supportive and positive, avoiding criticism/corrections.
- Pay attention to body language
- Ask the person to repeat if necessary, rather than pretending you understand.
Guidelines for communicating with the cognitively impaired client
Communication with the Cognitively-Impaired Client:
COGNITIVE:
DEMENTIA IMPAIRED
What is dementia? Dementia is a gradual decline in mental and social functioning compared to an individual’s previous level of functioning. A client may have memory loss, personality change, behavior problems, and loss of judgment, learning ability, attention, and orientation to time and place and to oneself. Alzheimer’s disease is the most common cause of dementia, and we will spend more time on this as it will likely be one of the more frequent causes of cognitive impairment of residents in your facility.
Alzheimer’s disease is a chronic, progressively debilitating illness. At first the symptoms are mild and might include difficulty remembering names and recent events, showing poor judgment and having a hard time learning new information. At this early stage, the person often tries to deny their problems. Most difficulties at this time are with performing IADLs.
As the disease progresses, the person is unable to judge between safe and unsafe conditions and will need help to dress, eat, bathe and make decisions. There may be personality changes such as increased suspiciousness. Unfamiliar people, places, and activities can cause confusion and stress. The person shows less interest in others and wants to withdraw to familiar, predictable surroundings and routines. The person in later stages has difficulty performing basic ADLs.
Some common behaviors associated with Alzheimer’s disease are rapid mood changes, crying, anger, pacing, wandering, doing things over and over, asking the same question, following people closely and inappropriate sexual behaviors.
Cognitive impairment refers to difficulty in processing information. There are numerous diseases that cause cognitive impairment, such as Alzheimer’s, Parkinson’s, Multi-Infarct Dementia, and AIDS. All of these diseases affect the brain in different ways to cause impairment. Care recipients with any of these conditions will require unique caregiving in order to deal with some of the problems present. The symptoms presented will vary from person to person and will depend on the stage of the disease. Some of the common symptoms associated with dementia are as follows, with some examples:
- Gradual memory loss
- Inability to perform routine tasks–dressing, cooking, cleaning
- Disorientation in time and space – don’t know what day it is or where they are
- Personality changes
- Unable to learn new information
- Judgment is impaired – doesn’t know if something is safe or is unable to make choices
- Loss of language skills – can’t remember words, etc.
Much of the time care recipients with cognitive impairment do not know what they are doing or saying. They have little control over thoughts or behavior. You usually cannot change the care recipient and, instead, must change how you react. This is the most important thing to remember.
- The care recipient is not asking you the same question over and over and over to annoy you.
- The care recipient does not remember and that is why the question is repeated.
Continue to answer the questions. Look for possible reasons for the repeated questions, such as the need for reassurance, acceptance, or love. Another way to look at this type of behavior is this – to the care recipient, there is no past and no future, but only the immediate present.
Cognitive impairment (cognition means of or relating to conscious thinking) is a term that simply means someone has lost a large amount of his/her higher intellectual ability. What do we mean when we use the term higher intellectual ability? We mean the ability to think and reason, the ability to use logic. We mean the ability to communicate and the power of memory. We mean all of the mental capacity that we need in order to function as human beings in our daily lives People with cognitive impairment have difficulty in communicating. They have difficulty understanding what is said to them. They can, at times, become confused about who you are, and they can be confused about who they are. They can be confused about where they are, what day of the week it is, and what year it is. People who suffer from cognitive impairment do not have the ability to think clearly and logically or they may only be able to do so once in a while. There is no one single condition, illness, or disease that causes cognitive impairment. People with cognitive impairment may have had a stroke, they may be suffering from Alzheimer’s disease, they may have had a head injury, or it may not be known why they have lost the ability to be rational. The only certainty is that there has been some illness, disease or accident that has permanently damaged the parts of the brain that control the ability to think, concentrate, and reason.
Although many people with cognitive impairment are elderly, being old does not always mean that someone has a diminished mental capacity. But regardless of why your clients have a cognitive impairment, coping with this situation can be very difficult. It takes patience and compassion. Above all, as a health care professional, you must remember that these patients do not have the ability to function and think as you do. We use our powers of thought, concentration, memory, logic, and language to cope with the world around us. For these people, those skills are absent or severely damaged. As a result, they cannot understand what they see and what you say. Many times, this will leave them frightened and confused. And more importantly, it leaves them dependent on you as a professional.
And the confusion and difficulty in communicating with these clients can be quite frustrating. So, make no mistake about it: working with a client who has a significant degree of cognitive impairment can often be very difficult. However, it is important to realize that these interactions are a two-way street; the situation is difficult for the client, as well. So when you are caring for someone who is confused, uncooperative – perhaps even aggressive – it is absolutely natural to feel frustrated. But remember: the client is doing the best he/she can and their feelings of confusion and fear are probably just as intense as your feelings of frustration.
A PRACTICAL APPROACH TO WORKING WITH CLIENTS WHO HAVE COGNITIVE IMPAIRMENT, fortunately, with the proper attitude and some simple techniques, working within these situations doesn’t have to be painful for you or your clients. Here are some basic tools that can help you when you are working with a client who has cognitive impairment.
Patience: You will need a lot of patience. The natural instinct when interacting with another adult is to assume that he/she is at your level of emotional and intellectual ability. This is not true of the client with cognitive impairment. This is a simple idea to understand, but many people have difficulty remembering this.
Non-verbal communication: Most of us think of communication as we say or the words we use. But much of our communication is non-verbal. The tone of your voice, the loudness or softness of your speech, the speed at which you talk, the way you stand, and where you stand when you speak to someone – all of these are forms of non-verbal communication. People with cognitive impairment may have lost the ability on an intellectual level to understand what you are saying. But their other senses are completely intact. They will, often, respond to how you speak to them rather than what you are saying. It is often best to stand where the person can easily see you. Making eye contact is important. Avoid touching the person until you are sure he/she won’t feel threatened by physical contact. Never pull or yank on someone if you want that person to move, change positions, stand up, etc. When you first approach someone, try and do so slowly; don’t rush at them.
Verbal communication: You don’t have to be talked down to these people. However, until you have established otherwise, it is sensible to be gentle when talking to these clients. Speak slowly and clearly. Try and keep your language at a basic level. Give them time to process what you are saying, and try and remember that it may take them far longer than you imagine to completely grasp the meaning of what you have said. It also helps to keep your communication simple and direct. Don’t be afraid to repeat what you have said, and don’t be surprised or frustrated if you have to. And don’t forget: although you may remember something that was said to you earlier in the day or earlier in the week, these clients may forget something that was said to them just an hour ago. Constant repetition and reinforcement will help clients to remember. Do not speak quickly, and make sure that you use simple language…
Flexibility: Perhaps nothing is more important when working with a client who has cognitive impairment than flexibility (And the opposite is also true: nothing is more harmful when working with these clients than being stubborn or rigid). What do we mean when we use the term flexible? It means simply that you adjust to the demands of the situation. It means that you are able to change your plans. It means that you realize what is/isn’t important, and that you know that getting the task done is far more important than how you do it.
Priority setting: All too often, health care professionals see their job as a series of tasks that need to be accomplished. That is true, but working with people is very complex. Many times it is simply not possible to do everything you need to do and want to do in the way you want to and when you want to. Situations change and people change. If you are not able to clearly see what, at any given time, is the most important priority, your job will be very difficult. Ask any experienced health care professional and he/she will tell you: in order to function efficiently, it is very important to know and decide what is most important, but you also need the ability to see that the situation has changed and to understand that a new, more important priority has replaced the previous one.
Regular routines: Because the person with cognitive impairment has difficulty remembering people, places, and situations, he/she can be helped by establishing reliable routines. If it is possible, try and arrange for the same PCW to work with the same clients. Try and find a routine for daily activities that are simple, do not change, and will be easy to remember for the client. Be careful to slowly introduce changes into the client’s daily routine, and try and explain these changes as clearly as possible. And if you tell the client that you are going to do something, make sure that you follow through on your promise. The client may surprise you by remembering what you said (e.g., you will in his/her home at 9 in the morning to help them get dressed) and may become disoriented if you do not keep your word. Example: Imagine that you need to assist a client in getting out of bed and getting dressed. You are very busy and you have a lot of other things you need to do for other clients, as well. But the client you are working with is resisting all of your efforts. He doesn’t want to get up, and he doesn’t want to get dressed. You can’t understand why, and he can’t tell you. You can try and force the issue, but when you do, he begins to get agitated. You need to determine what the most important priority is, and what the best way to accomplish that goal is. Perhaps in this situation, you have more time than you think. You might be able to sit quietly with this person for a bit and give the person a few minutes in which to adjust. Perhaps you can accomplish the task in steps; this will also give the client time to adjust. Also, you might be able to move to another task with another client. It may not be important – really important – that the client gets dressed right at that time you had planned. Always ask yourself: Can you change your priorities to make your day and the clients run a bit smoother?